Post-COVID-19 Disease Surveillance and Tracking: Lessons from Ethiopia’s Digital Health Response
March 19th, 2021 | viewpoint
On March 13, 2020, Ethiopia confirmed its first COVID-19 case. As of February 24, 2021, the government’s official count of COVID-19 cases was 155,234, with 2,316 reported deaths. The Government of Ethiopia and its partners’ concerted response to COVID-19 has led to considerable improvements. COVID-19 testing capacity has been expanded and screening, isolation, and treatment centers have been established and operationalized across the country. Community-based outreach services have been enhanced and the public health emergency management information system, which is integrated in the DHIS2 routine health information management system, has been strengthened to address COVID-19.
Despite these efforts, the pandemic has created a significant disruption in the use of essential health services because of supply and demand constraints. For example, on the supply side, the health workforce faces challenges resulting from many providers having contracted the virus and significant limitations in providers’ ability to use outreach services to reach vulnerable populations. On the demand side, some patients are unwilling to seek care from fear of becoming infected with COVID-19. This is compounded by many patients’ challenges paying for health care due to pandemic-related impacts on income and mobility.
Evidence-based decision-making and efficient and effective management of the COVID-19 response is at the heart of Ethiopia’s Emergency Preparedness and Response Strategic Plan. The MOH, in collaboration with USAID-funded Ethiopia Digital Health Activity and the Bill and Melinda Gates Foundation-funded Data Use Partnership (DUP) project, developed a national COVID-19 surveillance and tracking system. The system supports the enrollment and tracking of suspected cases; captures symptoms, demographics, risk factors, and exposures; and monitors patient outcomes. The DHIS2-based tool facilitates surveillance workflows and the automated analysis of key components of routine and active surveillance while leveraging WHO-recommended protocols, with multiple integrated data sources and applications feeding data into the main surveillance and tracking system. See Figure 1 for the digital platform architecture of Ethiopia’s COVID-19 response.
Data from these sources are used to prepare COVID-19 daily situation reports and presentations for the national task force and other leaders and to respond to data requests from a variety of stakeholders. In addition, a high-level analysis of the data collected through house-to-house surveillance activities has been regularly carried out.
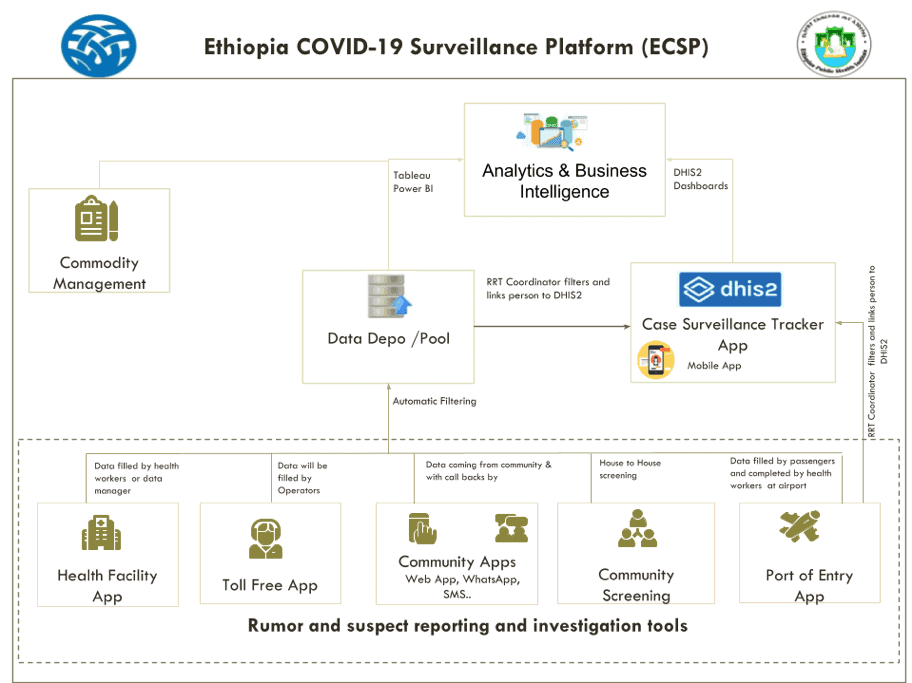
A port-of-entry (POE) health declaration system was developed and implemented to record residents’ personal identification information, including phone numbers, travel history, health symptoms, and geo-location. The forms are generated via QR codes at all POEs provide each traveler with a unique identification number or code. Screeners from the Ethiopia Public Health Institute (EPHI) will then digitally record every traveler’s temperature and include this information in the digital record used for 14-day monitoring and follow-up. It is assumed that travelers enrolled in the program who meet the suspected case definition (i.e., an asymptomatic traveler registered at a POE who later develops symptoms) will be enrolled in the COVID-19 case surveillance program. This application automates the country’s Traveler’s Health Declaration Form for Coronavirus Disease, a formerly paper-based form that passengers must complete when entering Ethiopia.
The MOH and its partners also developed and implemented a community reporting and investigation tool for rumored and suspected cases of COVID-19, which can also be used for self-reporting by symptomatic individuals. The MOH also has a call-capturing tool for the COVID-19 call center that provides information about where individuals can volunteer, request help, learn more about the pandemic, and report rumors. A CommCare-based community house-to-house screening system was also created to serve as a data collection tool and job aid for nationwide door-to-door COVID-19 screening campaigns. The Activity also developed and implemented a health facility reporting app, a toll-free recording app, WhatsApp and Telegram helplines, and an app for reporting and investigating rumored and suspected cases.
Numerous challenges have been encountered during the development, implementation, and end-user support processes for the COVID-19 surveillance and tracking system. Some challenges have been related to governance, in particular, the length of time that was devoted to selecting an appropriate platform, given the overwhelming number of solutions available for COVID-19 digital health responses. Additional challenges have included coordinating and aligning technical partners in support of the government’s response to the pandemic.
Other implementation challenges have resulted in poor quality surveillance data, including the recording and reporting of incomplete patient data from suspect investigation to determining outcomes, the absence of a unique ID number to track patients, difficulties in safely providing IT support in isolation and treatment centers, and health workers’ many competing priorities.
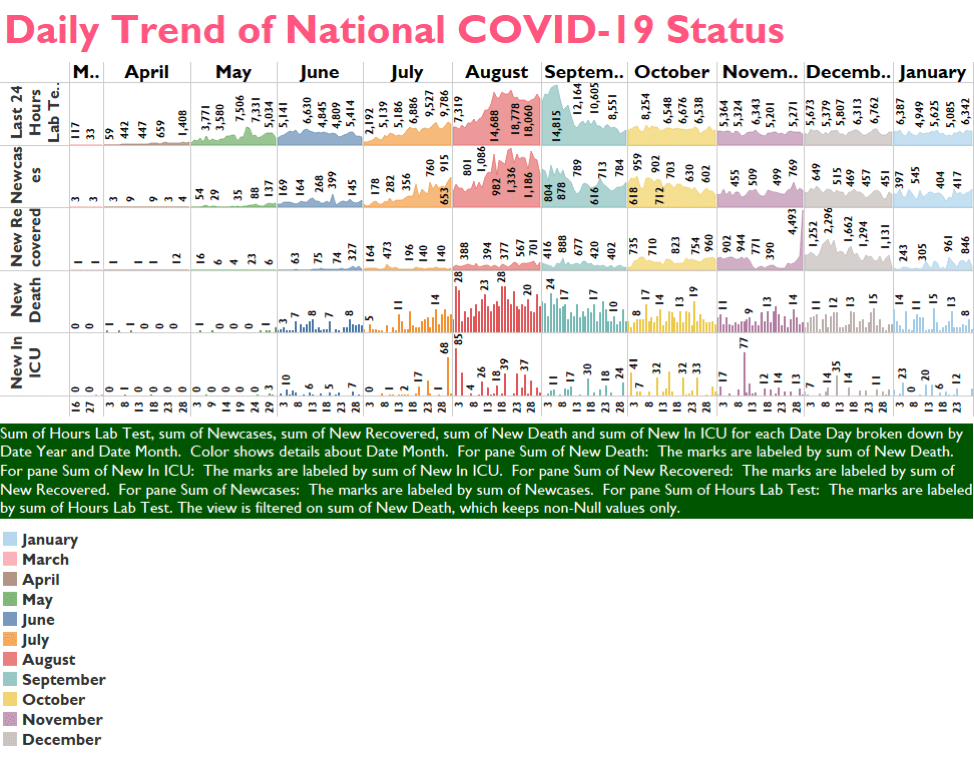
The practice of using surveillance and patient-level data for an evidence-based COVID-19 response has been low at national and subnational levels. There are efforts to develop a COVID-19 dashboard (see Figure 2) and generate evidence for various audiences. However, there is little evidence in terms of the actual use of the data for day-to-day decision-making.
Several lessons have been gained from Ethiopia’s COVID-19 surveillance and tracking system. First was the difficulty of finding a single platform or solution that met all of the country’s COVID-19 surveillance and tracking requirements. The DHIS2-based tracker described in this article responds to some but not all of the requirements of the National Emergency Operations Center. As a result, the MOH, EPHI, and partners needed to review existing tools in the national eHealth architecture to determine which were most appropriate for the pandemic and its associated use cases.
While the solutions identified provided a good foundation for the surveillance and tracking system, they required significant customization to meet local COVID-19 needs. In fact, one of the most important lessons from the Ethiopian surveillance and tracking system is the importance of local capacity to contextualize and customize global digital goods to ever-changing local requirements. In this case, the DHA, DUP, and others developed tools for local use to fill gaps in some of the global goods that were leveraged.
Ethiopia drew on existing digital health teams, human resources, and infrastructure to quickly deploy the surveillance and tracking system. The DHIS2, eCHIS, and LMIS technical teams were repurposed to customize the COVID-19 tracker, community screening, and COVID-19 commodity management tools, respectively. This approach resulted in the rapid customization and deployment of existing tools, the tapping of well-trained personnel, and leveraging an existing infrastructure developed for routine digital health surveillance and tracking.
Another significant lesson has been the importance of Ethiopia’s continued investment in long-term disease surveillance while responding to the COVID-19 pandemic. The investment in the COVID-19 digital health response will prove particularly invaluable when the tools, capacity-building programs, and knowledge and skills strengthened during the response are employed for disease surveillance and patient tracking following this pandemic. Read on for more lessons learned from the COVID-19 response.
We strive to build lasting relationships to produce better health outcomes for all.