Maintaining TB Testing During COVID-19 in Northern Uganda
March 25th, 2022 | story
The COVID-19 pandemic caused widespread disruptions to health service delivery. In particular, it arrested progress on ending TB in high-burden countries like Uganda, achievement of the 2018–2022 United Nations High-Level Meeting targets on TB treatment and prevention, and the WHO objective of ending the TB epidemic by 2035. As newer COVID-19 variants continued to devastate many low- and middle-income countries in 2021, the extent of these setbacks, especially in TB case identification, increased.
Tuberculosis is the leading cause of death by infectious disease in Uganda. According to the Ministry of Health, which in November 2019, declared TB a public health emergency, it kills 30 Ugandans every day. Lango, Acholi, and Karamoja Regions in northern Uganda were chosen to lead the emergency plan because they have the highest prevalence of TB. However, the implementation of the emergency plan was disrupted by the COVID-19 pandemic, and subsequent restrictions interrupted the continuity of TB services, including community outreach, screening, and testing at health facilities.
The USAID-funded Regional Health Integration to Enhance Services-North, Lango (RHITES-N, Lango) project supports the Ministry of Health through the National TB and Leprosy Program to establish high-quality TB diagnosis and treatment services and control activities in the Lango Sub-region of northern Uganda.
“During the first months of the pandemic, TB notifications decreased sharply,” says Joseph Nturo, laboratory advisor for the project. “The restriction in movement, fear of contracting or being misdiagnosed with COVID-19, and stigma all hindered care-seeking.”
To ensure continuity of TB services, the project supported systematic contact tracing; hotspot and door-to-door screening; training lay health workers on basic TB facts; and use of intensified case-finding guides, presumptive case registers, infection control and sputum collection techniques, and community drug refills.
The project also engaged community support organizations, village health teams, and community linkage facilitators to reach marginalized and remote populations, and strengthened access to diagnostics (X-rays, GeneXpert, and TB LAM tests). The combination of approaches sustained TB case identification, particularly through GeneXpert.

GeneXpert Testing
“The GeneXpert is a widely accepted rapid diagnostic tool for early detection of mycobacterium TB and rifampicin [TB drug] resistance,” says Joseph.
Lira Regional Referral Hospital Lab serves the nine districts and one city of Lango. It had one four-module GeneXpert machine for TB tests that, when COVID-19 arrived, could not run all the tests in a timely manner.
“We were overwhelmed by COVID-19,” says Geoffrey Achillam, lab technologist at the hospital. “At the peak of the Delta variant, in a day, we would test more than 600 COVID-19 samples,” he adds.

Because COVID-19 results were needed quickly to isolate people who tested positive, the hospital prioritized COVID-19 over TB testing. This dramatically reduced the turnaround time for the release of results and treatment for TB clients. In response, RHITES-N, Lango, through the Ministry of Health, supported Lira Regional Referral Hospital to acquire a 16-module GeneXpert machine. The project also upgraded the hospital’s backup power system to accommodate the new machine, and installed the software and trained lab personnel to operate it.
“The new machine meant that we could efficiently run 16 tests simultaneously,” which improved turnaround time for both TB and COVID-19 results, says Geoffrey.
As COVID-19 subsides, the hospital is experiencing a surge in TB tests, as shown in the figure below.
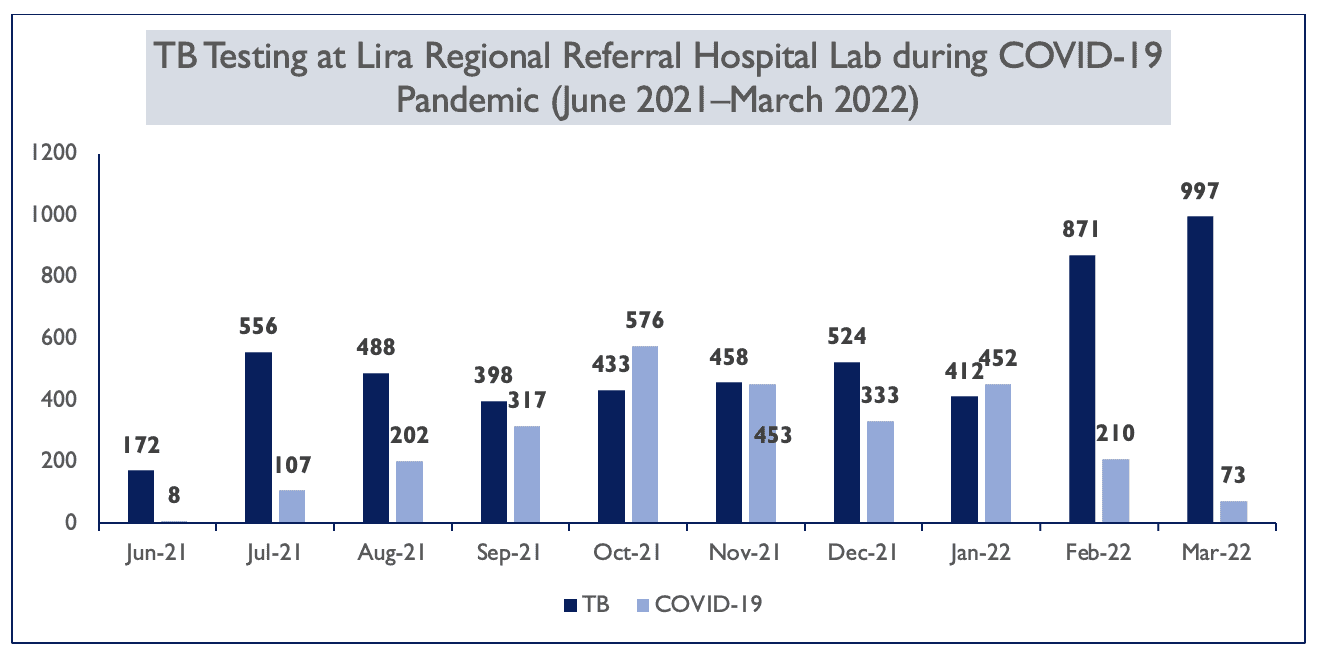
After Kampala Region, Lango has the second-highest drug-resistant (DR) TB case notification rates in Uganda. The RHITES-N, Lango project continues to support DR-TB services to improve diagnostics of rifampicin-resistant cases, and increase GeneXpert access for pulmonary bacteriologically confirmed cases by ensuring all samples are transported to and tested at the 12 GeneXpert facilities in the region. Most importantly, the project is working toward the national target of improving treatment outcomes to 80 percent of cases.
Written by Angela Kateemu
We strive to build lasting relationships to produce better health outcomes for all.