This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognizing you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
Engaging Civil Authorities and Local Leaders for
Vaccinating every child, every year, is a tremendous undertaking for health systems across the globe. While 116 million children were vaccinated worldwide in 2018, another 20 million went unprotected from vaccine-preventable diseases. Vaccinating all children, every year, requires support at all levels, from global partners to national governments to district-level stakeholders who decide on funding allocations vital to last mile delivery of immunization services.
Photo: Kate Holt
While the cost of vaccines and refrigerators are often covered by national budgets, it is the provision of resources at local levels to cover program operation costs that often make or break the success of immunization.
These costs include transportation for health workers who travel long distances to provide vaccination services in remote communities.
Photo: Adriana Almiñana
Other program costs include data management supplies such as monitoring charts, child health registers, and home-based records, which health workers use to track progress toward vaccinating every child and determine which families and communities have not been served.

Civil authorities and political leaders at district and local levels often determine funding for these operational costs.
Collectively referred to as “non-health stakeholders,” they have a key role in supporting the vaccination of all children. They can provide financial and in-kind support for services and use their voices to increase community trust and demand for immunization.
In Ethiopia and Uganda, JSI has helped health managers collaborate with non-health stakeholders to solve persistent local funding and support problems.
Photo: Adriana Almiñana
Improving access to services in remote communities in Ethiopia
Itang District in Gambella Region is home to diverse and dispersed communities, many of which lack access to health services. Immunization outreach sessions to these areas were cancelled frequently because of budget constraints.
Over the course of several months, JSI helped district health managers calculate how many outreach sessions would be needed and at what cost, and built their capacity to advocate for funding from local civil administrators.
The district health managers used these data and their strengthened advocacy skills to appeal to the civil administrator, who agreed to fund 156 outreach immunization sessions to vaccinate Itang’s children.
Photo: Adriana Almiñana
Working with non-health stakeholders in Uganda to remove “last-mile” bottlenecks
In Uganda, JSI has involved non-health stakeholders in immunization and built health personnel capacity to communicate with them. These efforts have increased financial, in-kind, and social/political support for routine immunization in more than 25 districts.
In Bulambuli district, involving civil and administrative authorities in mapping and microplanning helped reveal that more than 50,000 people lacked access to health facilities. JSI built health officials’ capacity to work with non-health stakeholders, which led to the repurposing of unused public buildings as six new health facilities, doubling the reach of immunization and other basic health services from 340 to 695 villages.
In Kanungu district, a clinic director realized that the lack of transportation at his facility was hindering provision of immunization in distant communities. When he appealed to a local community bank for support, it agreed to pay 75% of the cost of a new motorbike if the clinic could come up with the rest. It did, and the motorbike allowed clinic staff to reach all its service areas and eventually double its rates of initial use of vaccination services.
Photo: Kate Holt
Such efforts prove that there are financially and politically viable local solutions to vaccinating last-mile children.

Photo: Kate Holt
It is this shared commitment between people within and beyond the health system that will help us reach everyone with high-quality, life-saving immunization services.
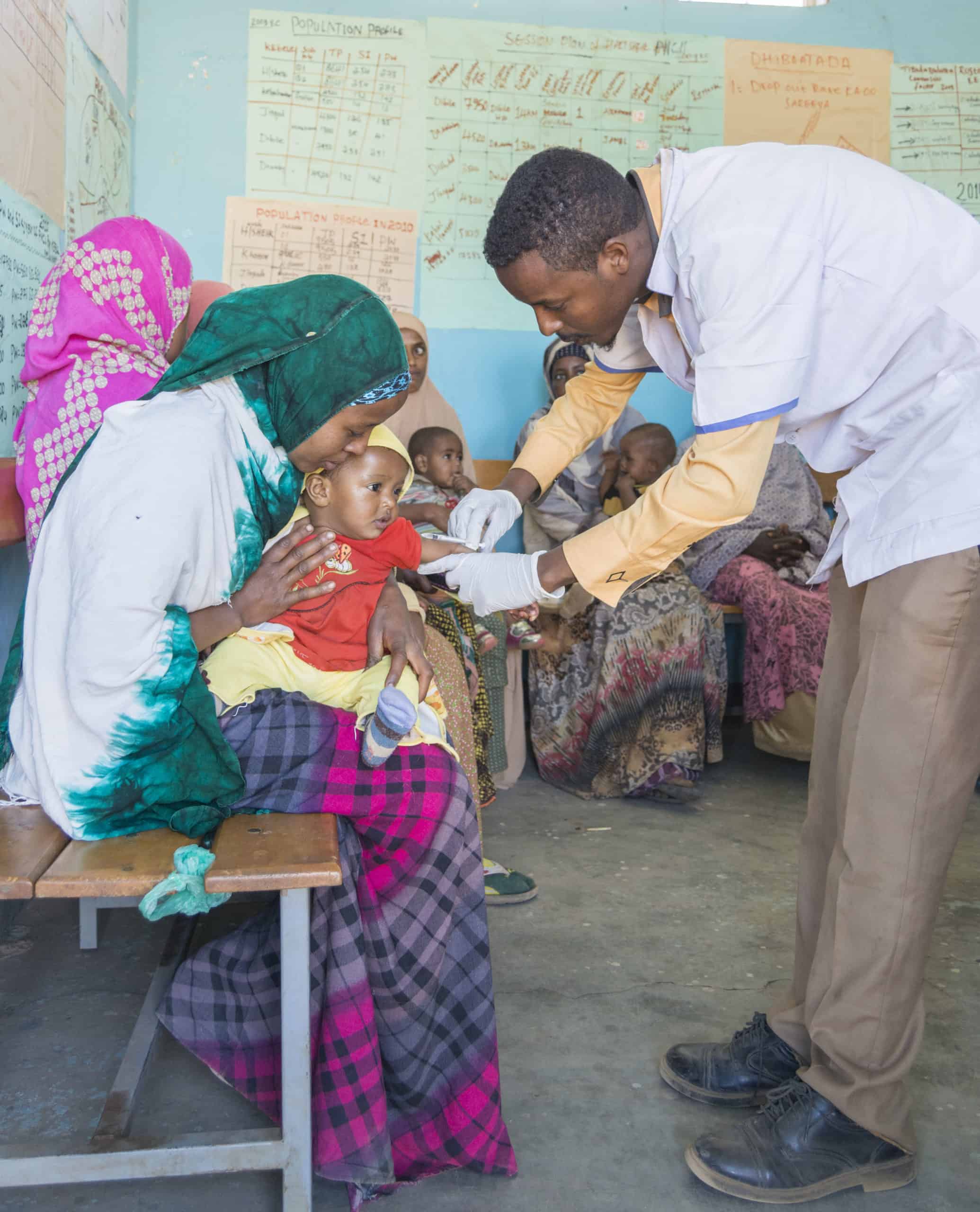
Photo: Natasha Kanagat

